Chronic Kidney Disease (CKD) affects approximately 10 percent of the global population and is characterised by gradual renal function loss leading to severe morbidity and mortality (Yoga et al, 2015). Haemodialysis (HD) remains the most common renal replacement therapy, yet it is associated with numerous physical and psychological complications. Among these, muscle cramps, reported by 33-86 percent of HD patients, are one of the most distressing symptoms (Punj et al, 2020; Daugirdas et al, 2015). These cramps arise due to electrolyte imbalances, rapid fluid shifts, altered muscle metabolism, and neuromuscular dysfunction (Hill et al, 2016). Such discomfort interrupts dialysis sessions, reduces treatment adherence, and deteriorates patients’ Health-Related Quality of Life (HRQoL) (Reiner et al, 2013).
Progressive Muscle Relaxation (PMR), developed by Jacobson involves systematic tensing and releasing of muscle groups to promote relaxation and reduce muscular tension. Studies demonstrate PMR’s effectiveness in managing anxiety, fatigue, and muscular pain among chronic illness populations (Ghasemi et al, 2016; El-Nahas, 2021). However, limited evidence exists regarding PMR’s specific role in alleviating dialysis-induced muscle cramps in the Indian population.
Considering the high prevalence of cramps and their impact on adherence and mental health, there is a pressing need for low-cost, evidencebased, nurse-deliverable interventions. Hence, this study evaluates the effectiveness of PMR on muscle cramps and quality of life among CKD patients on haemodialysis, addressing a critical research gap in non-pharmacological symptom management.
Objectives
This study was set out:
1. To assess the effect of Progressive Muscle Relaxation on the severity of muscle cramps in patients undergoing haemodialysis in the experimental group.
2. To evaluate the impact of PMR on the quality of life of patients receiving haemodialysis in the experimental group.
3. To compare the post-intervention outcomes of muscle cramps and QoL between the experimental and control groups.
Review of Literature
A systematic search was performed using PubMed, Google Scholar, and Scopus with keywords: Progressive Muscle Relaxation, haemodialysis, muscle cramps, and quality of life. Studies published between 2010–2024 were reviewed.
Evidence consistently reports that PMR reduces anxiety, fatigue, and muscular discomfort across chronic disease populations (Jones et al, 2019; Tsai et al, 2007; Chang et al, 2020). Ghasemi et al (2016) found that PMR improved sleep and reduced fatigue in CKD patients, while El-Nahas et al (2021) demonstrated its benefits for neurological symptoms during dialysis. Jones et al (2019) confirmed a significant reduction in muscle cramp frequency following PMR training.
Research gap identified: Despite these promising outcomes, Indian studies assessing PMR’s impact on HD-induced cramps are scarce, emphasising the need for region-specific evaluation and integration into nursing practice.
Materials and Methods
It was a quasi-experimental study in which pre-test–post-test control group design was adopted. The study was conducted at Muljibhai Patel Urology Hospital, Nadiad, Gujarat. The sample consisted of 60 CKD patients undergoing maintenance haemodialysis, selected through non-probability convenience sampling, equally divided into experimental (n=30) and control (n=30) groups.
Inclusion criteria:Adults aged 18 years or more, diagnosed with CKD, undergoing HD for at least six months, able to follow instructions, and willing to participate were included.
Ethical consideration:Ethical clearance was obtained from the Institutional Ethics Committee, and written informed consent was taken. The tool’s validity was established by expert review and pre-testing.
Data Collection Tools
A. Socio-demographic profile
B. Modified muscle cramps questionnaire – categorising cramps as mild (1-5), moderate (6- 11), and severe (12-17).
C. WHOQOL-BREF, covering physical, psychological, social, and environmental domains.
Procedure: PMR sessions were administered three times weekly for four consecutive weeks, each lasting 20-25 minutes, guided by the investigator during HD sessions. Quality of Life and muscle cramp assessments were conducted before and after four weeks of intervention.
Data Analysis: Data were analysed using SPSS software, employing descriptive statistics for demographics and paired and independent t-tests for comparing pre- and post-intervention results. A significance level of p < 0.05 was used.
Results
The sample characteristics of the study population revealed similarity between the experimental and control groups. The majority of participants were in the age range 39-48 years and over 49 years, with a predominantly male gender distribution (around 70%). Both groups also shared a high proportion of Hindus (87%) and primary-secondary education (40%).
Family structure leaned towards joint families (67-77%), with income (in Rupees) mainly between 10,000 and 30,000. Residence was split relatively evenly between rural and urban areas (40-43% each). Regarding health factors, the most common illness duration was 6 months to 1 year (33-43%), and a significant majority experienced frequency of haemodialysis (3 cycles per week) in both groups (by 87-97%).
Effect of PMR on muscle cramp severity is shown in Table 1 and Fig 1. Hypertension emerged as the dominant co-morbidity, affecting around 50-60 percent of participants in each group.
Table 1: Effect of PMR on muscle cramp severity -
Experimental group (within group) (n=30)
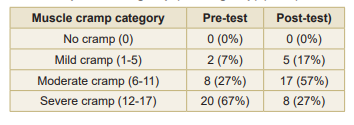
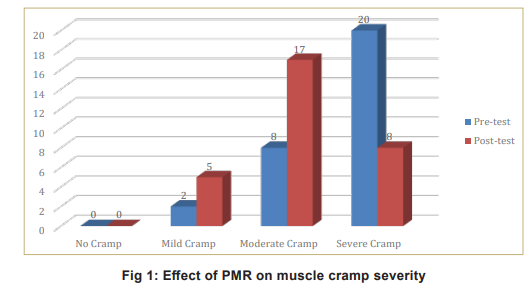
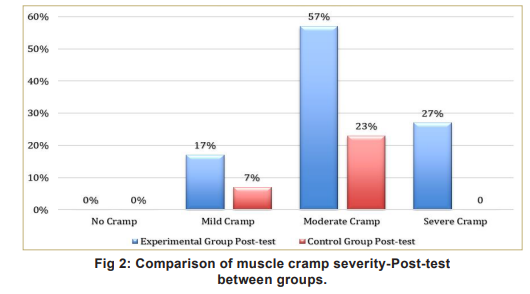
In the experimental group, PMR reduced the proportion of participants experiencing severe cramps from 67 percent to 27 percent, indicating a significant alleviation of muscle cramps (Table 2). PMR significantly improved overall QoL among participants, with a mean increase of 48.97 (t=11.89, p<0.0001). Post-test comparison of muscle cramp severity between groups is shown in Table 3 and Fig 2.
Experimental group showed significant reduction in severe cramps compared to control, demonstrating the efficacy of PMR in alleviating muscle cramps (Table 4).
The experimental group had significantly higher QoL scores than the control group post-intervention (t=31.78, p<0.0001), confirming the positive effect of PMR.
Before the intervention, 67 percent of patients in both groups experienced severe muscle cramps. After four weeks of PMR, the experimental group’s severe cramp incidence dropped to 27 percent, while control group cramps persisted (70%).
Quality of Life improved significantly in the experimental group (pre-test mean = 65.43 ± 22.17;
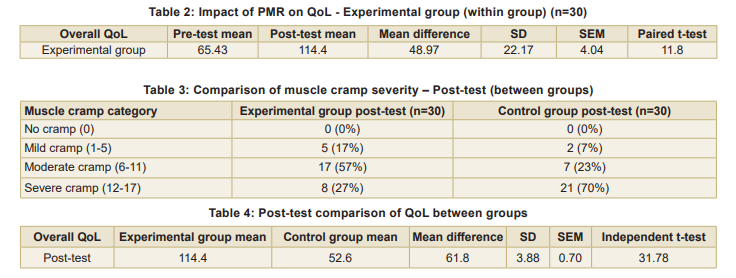
post-test = 114.4 ± 3.88; t = 11.89, p < 0.0001). Between-group analysis showed a post-test mean difference of 61.8 (t = 31.78, p < 0.0001).
These results clearly demonstrate PMR’s significant positive influence on both muscle cramp reduction and QoL improvement among haemodialysis patients.
Discussion
This study supports PMR as an effective, low-cost intervention to alleviate HD-related complications. The findings correspond with those of El-Nahas et al (2021), who observed symptom relief in restless legs syndrome among dialysis patients using PMR. Both, Ghasemi et al (2016) and El-Nahas et al (2021) also reported enhanced sleep quality and reduced fatigue post-intervention.
PMR improves neuromuscular coordination and psychological resilience, thereby enhancing HRQoL. These findings also align with Yildirim & Fadiloglu (2006) and López-Torres (2017), who highlighted relaxation’s role in improving emotional stability and coping among CKD patients.
Implications & Recommendations
Nursing Practice
Nurses should integrate PMR into routine HD care to relieve cramps and promote comfort. PMR can be administered during dialysis sessions to reduce symptom distress.
Nursing Education
Include PMR and similar mind-body interventions in nursing curricula and skill labs.
Nursing Administration
Policy-level inclusion of PMR in dialysis protocols and regular training of dialysis staff.
Nursing Research
Conduct longitudinal and multicentric studies to evaluate PMR’s long-term impact on QoL, adherence, and emotional health.
Study limitations:
The study’s constraints include a small sample size, single-centre design, and short-term follow-up. Further multicentre randomised controlled trials are recommended to generalise findings and assess long-term effects.
Conclusion
This study concludes that Progressive Muscle Relaxation (PMR) is an effective, safe, and feasible intervention that significantly reduces muscle cramps and improves quality of life among CKD patients undergoing haemodialysis. Its simplicity, cost-effectiveness, and suitability for nurse-led implementation make it ideal for incorporation into routine dialysis care protocols. Integrating PMR can enhance holistic nursing practice and reduce the overall morbidity burden of CKD.
1. Yoga R, Kaur S, Tan JA, Dass A. The prevalence and associated risk factors of muscle cramps among hemodialysis patients. J Ren Nutr 2015; 25(5): 364-70. doi: 10.1053/j. jrn.2015.03.005
2. Punj S, Enaam A, Marquez A, Atkinson AJ Jr, Batlle D. A survey on dialysis-related muscle cramping and a hypothesis of angiotensin II on its pathophysiology. Kidney Int Rep 2020; 5(6): 924-26. doi: 10.1016/j.ekir.2020.03.003
3. Daugirdas JT, Blake PG, Ing TS. Handbook of Dialysis. 5th edn, 2015. Philadelphia: Lippincott Williams & Wilkins
4. Hill NR, Fatoba ST, Oke JL, Hirst JA, O’Callaghan CA, Lasserson DS, et al. Global prevalence of chronic kidney disease: A systematic review and meta-analysis. PLoS One. 2016; 11(7): e0158765. doi: 10.1371/journal. pone.0158765
5. Reiner K, Tibi L, Lipsitz JD. Do mindfulness-based interventions reduce pain intensity? A critical review of the literature. Pain Med 2013; 14(2): 230-42. doi: 10.1111/ pme.12006
6. Ghasemi Z, Shahgholian N, Ebrahimi A. The effect of progressive muscle relaxation and aerobic exercise on anxiety, sleep quality, and fatigue in patients with chronic renal failure undergoing hemodialysis. J Nurs Res 2016; 24(1): 63-70. doi: 10.1097/jnr.0000000000000124
7. El-Nahas AM, Zayed B, Abd-Elbaset MA, Shaheen N. Progressive muscle relaxation for restless legs syndrome in patients on maintenance hemodialysis: A randomized controlled trial. Egypt J Health Care 2021; 12(1): 37-47. doi: 10.21608/ejhc.2021.167387
8. Jones LW, Eves ND, Peppercorn J, Courneya KS. Effect of PMR training on muscle cramps in CKD patients undergoing hemodialysis. J Ren Rehabil 2019; 21(3): 123-29
9. Tsai YC, Yeh SH, Tsai HH. The effects of exercise training on walking function and perception of health status in patients with peripheral arterial occlusive disease. J Nurs Res 2007; 15(4): 276-86
10. Chang CH, Lin CY, Mahat G. The effects of progressive muscle relaxation training on hemodialysis patients: A randomized controlled trial. Int J Nurs Stud 2020; 102: 103463. doi: 10.1016/j.ijnurstu.2019.103463
11. Yildirim YK, Fadiloglu C. The effect of progressive muscle relaxation training on anxiety levels and quality of life in dialysis patients. EDTNA/ERCA J 2006; 32(2): 86-88. doi: 10.1111/j.1755-6686.2006.tb00457.x
12. López-Torres I, Higueras P. Effectiveness of physical exercise and relaxation in controlling anxious and depressive symptoms in hemodialysis patients. Enferm Nefrol 2017; 20(1): 56-62

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.